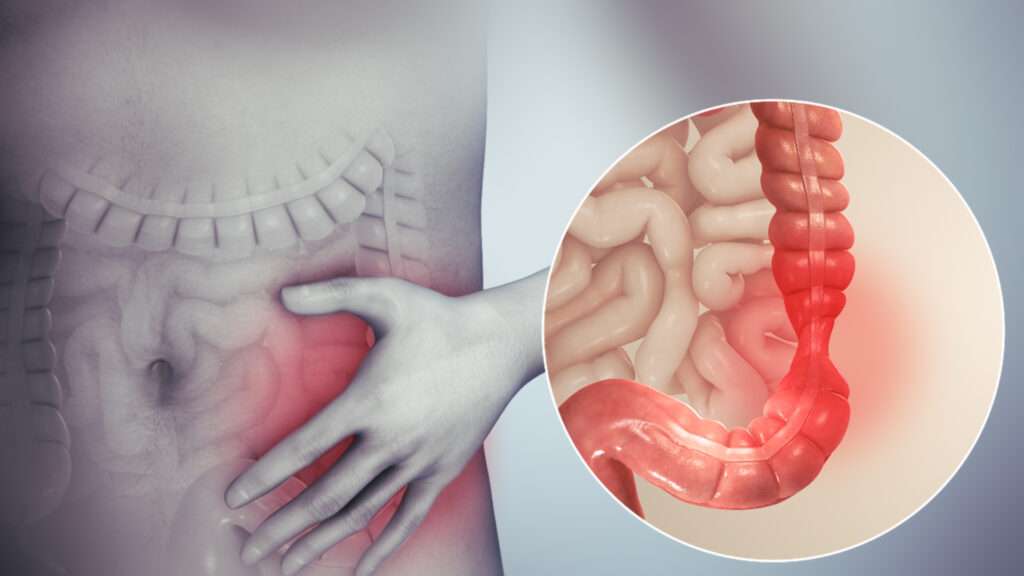
Irritable Bowel Syndrome (IBS) is a common gastrointestinal disorder that affects the large intestine (colon) and can cause a variety of digestive symptoms. It’s important to note that IBS is a chronic condition, and while it can be uncomfortable, it doesn’t lead to more serious conditions like inflammatory bowel disease or cancer. Here’s an overview of IBS
Symptoms: The symptoms of IBS can vary widely from person to person, and they may come and go over time. Common symptoms include:
- Abdominal Pain and Cramping: These are often relieved by having a bowel movement. The pain and cramping can range from mild to severe.
- Bloating: Many people with IBS experience bloating, which is a feeling of fullness or swelling in the abdomen.
- Gas: Excess gas production is a common symptom of IBS and can contribute to bloating and discomfort.
- Diarrhea: Some individuals with IBS primarily experience diarrhea, which is characterized by frequent and loose stools.
- Constipation: Others may primarily experience constipation, which involves infrequent bowel movements and difficulty passing stools.
- Alternating Symptoms: Many people with IBS experience a combination of diarrhea and constipation, with symptoms alternating between the two.
- Mucus in Stools: Some individuals may notice mucus in their stools.
Causes: The exact cause of IBS is not fully understood, but it’s believed to involve a combination of factors:
- Abnormal Gut Contractions: People with IBS often have abnormal contractions of the colon, which can lead to pain, gas, and changes in bowel habits.
- Nervous System Abnormalities: The communication between the brain and the gut is disrupted in people with IBS, leading to heightened sensitivity to pain and changes in bowel movements.
- Intestinal Inflammation: Low-grade inflammation in the intestines might play a role in some cases of IBS.
- Triggers: Certain foods, stress, hormonal changes, and infections can trigger or worsen IBS symptoms.
Diagnosis and Management: IBS is typically diagnosed based on symptoms and by ruling out other conditions. There’s no specific test for IBS, but a doctor might perform tests to ensure there are no underlying issues.
Managing IBS involves a combination of strategies:
- Dietary Changes: Identifying and avoiding trigger foods can help manage symptoms. Common triggers include certain types of fiber, caffeine, dairy, and fatty foods.
- Stress Management: Stress can exacerbate IBS symptoms. Techniques like meditation, and deep breathing can help manage stress.
- Medications: Depending on symptoms, doctors might prescribe medications to control diarrhea, relieve constipation, reduce muscle spasms, or manage pain.
- Lifestyle Modifications: Regular exercise, adequate sleep, and staying hydrated can help manage symptoms.
- FODMAP Diet: Some people with IBS find relief by following a low FODMAP diet, which involves avoiding certain types of carbohydrates that can contribute to symptoms.
It’s important to work with a healthcare professional to develop a personalized treatment plan for managing IBS. While IBS can be chronic, many people are able to find ways to effectively manage their symptoms and improve their quality of life.